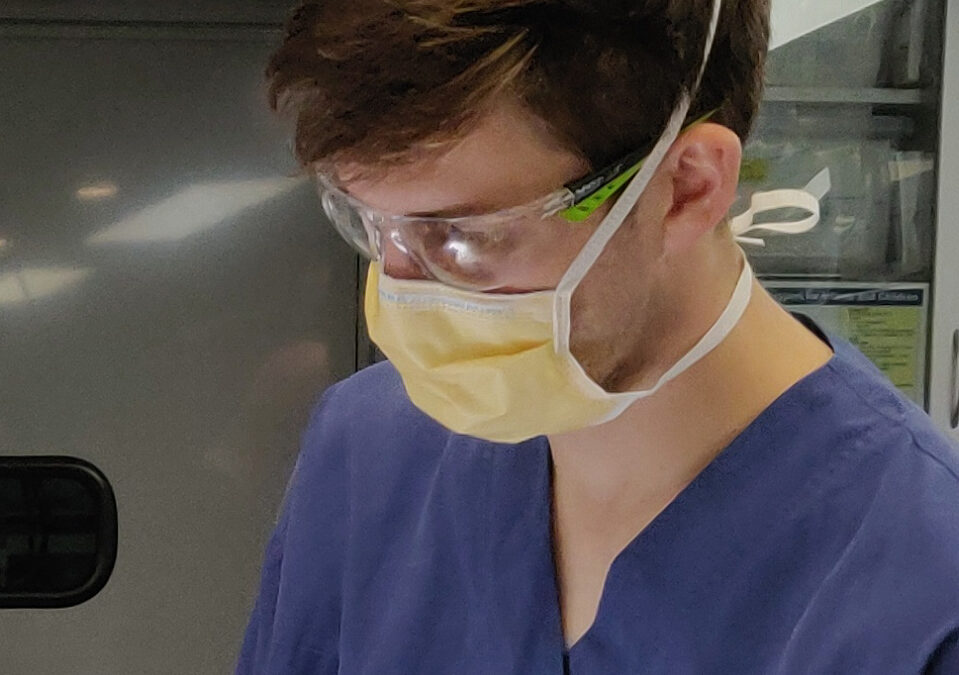
Rarely do high school students know what they want to do when they grow up, but when Tim Colson spent time aboard the Mobile Surgical Unit – Te Waka Hauora back in 2014 while in school, the seed was already planted that his future was going to be in medicine.
Tim (pictured above and below left) was only one of two school students in the south Canterbury area offered a chance to visit the surgical unit for one week as part of the Programme Incubator – a Hawke’s Bay District Health Board initiative, which introduces students to careers in the health sector. The programme included a trip to Timaru hospital where the students could engage directly with surgeons, nurses and other health professionals. Tim recalls learning about how a surgical theatre works and the different roles people have to ensure the theatre is running smoothly.
“Each specialty would tell me a bit about what they did, and why they chose their profession,” Tim begins. “I really enjoyed seeing what medicine and surgery looked like in practice. There is such a balance between knowing about the body and diseases, as well as the specific practical aspect. Even though most of it went over my head, I found the learning so interesting and is something that I wanted to learn more about.” Suffice to say, the experience directly contributed to his decision to pursue a career in medicine.
Fast forward to September 2020 and Tim was back at the place where it all began. This time working on the mobile surgical unit as part of his elective as a 6th year medical student, and in his final year of study at the University of Otago, Wellington studying Bachelor of Medicine and Surgery. He says exposure to rural medicine while also improving his surgical skills and knowledge were some of the reasons for revisiting the surgical unit. “Having spent time on the surgical unit prior to starting my degree, I thought it would be a fitting way to finish it off.”
Tim boarded the surgical unit in Christchurch to begin his training and embraced his hands-on role for five weeks; learning to adapt to different theatre situations and working alongside various health professional teams who have a plethora of knowledge to share, and who were happy to share it. Through conversations with knowledgeable and skilled clinicians onboard, which changed by the day, he listened to personal experiences, learnt different approaches to solving problems, as well as building awareness of what is involved in a career in medicine.
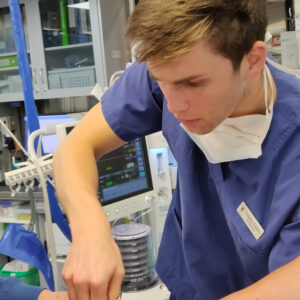
He says his experience was enriching and engaging and appreciated the encouragement from experienced staff. “The positive environment on the surgical unit makes it easy to get involved,” he says. “I learnt a lot from the anaesthetic side of working on the surgical unit. Having not spent a lot of time in this area I picked up a lot of practical skills, as well as heaps of the theory of the dynamic physiology. Having a variable schedule meant having a different discipline of surgery and this meant having to put on a different thinking cap.”
“One take away from my time with the surgical unit is the importance of improving access to health care in rural communities. I know in my future practice I will look at ways of improving this area of health inequity. Who knows, I may even work as a doctor on the surgical unit!”
And Tim didn’t shy away from giving a helping hand to the “steerologist” (driver) who was impressed with his enthusiasm for all aspects of the surgical unit, including assisting staff beyond the operating theatre. “Tim was busy from the start till end of day and did everything we asked and more – he will be a top doctor,” Gavin Hurring, steerologist says.
Anne Shirtliff, clinical nurse leader says “Medical students get real value out of working on the mobile surgical unit because they get an understanding and awareness of what it is like to work within a team and how important everyone’s role is to facilitate a smooth and safe patient journey.
“Students are expected to be part of the team and help in all roles when required, such as cleaning, making the beds, helping with pushing the bed or wheelchair to the hospital and helping the drivers with the pack-up chores at the end of the day.”
She says students receive consistent teaching and they can practice their newfound skills repeatedly, such as cannulation, intubation, management of airways, scrubbing, assisting in surgery and suturing. “You can see the students growing in confidence as each day goes by. Students are exposed to a variety of surgery and techniques and have the chance to ask many questions from the specialists, which may influence their future path.”
The purpose-driven student training on the surgical unit proves to be rewarding, fulfilling and fosters and exercises active thinking and leadership. Students engage in a series of conversations with different members of the clinical team to attain impactful insights and this helps students achieve higher levels of growth and engagement.

Pictured above: The team working on the mobile surgical unit during Tim’s five-week training (L-R) Jason Irwin, nurse, Bev Larson, anaesthetic technician, Sue Hooper, dental assistant, Garth Forbes, dental surgeon, Hugh Rorrison, anaesthetist, Wendy Lorentz and Tim Colson, medical trainee (below centre).
About Mobile Health
Mobile Health works in partnership with the Ministry of Health, local district health boards and your local health professionals to provide low risk, elective day surgery for rural New Zealanders. The service has been operating since March 2002 and since then has treated up to 30,000 patients, primarily in rural New Zealand.
Medical students continue to take advantage of the opportunity to work onboard the mobile surgical unit to get real-life insight into a theatre environment. They become part of a highly valued team and are encouraged to get involved in all aspects of theatre work. As part of their experience, they travel to various locations and develop a better understanding about the delivery of health care services to rural communities and the challenges they face.