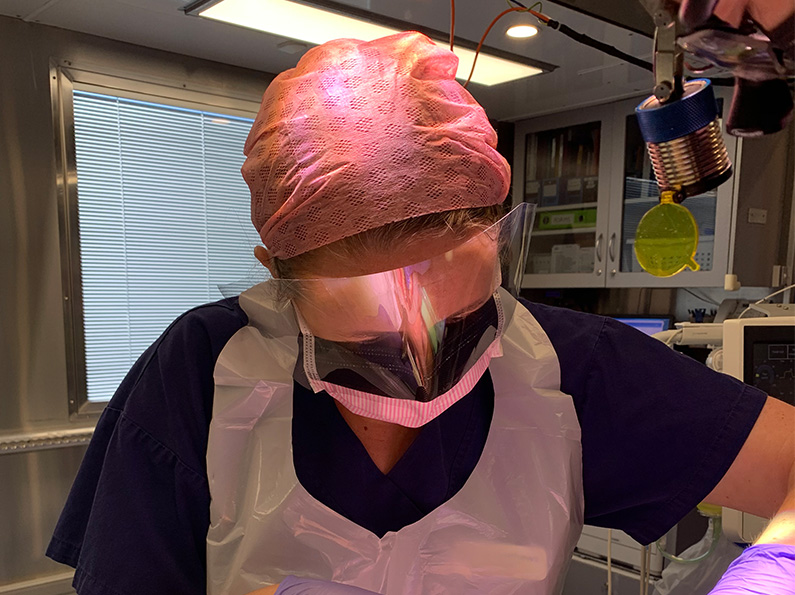
(Pictured above: Rachel Matthews assisting the dentist on the mobile surgical unit)
Rachel Matthews is a medical student studying in Timaru and worked on the Mobile Surgical Unit – Te Waka Hauora as part of her Trainee Intern Elective for her final year of medical school. She is one of many students who have had the opportunity to have hands-on experience working alongside doctors and nurses to learn all aspects of surgical care including admission, anaesthetic care, surgical procedures, and recovery. Working on the unit for four weeks also allowed her to travel to rural communities across New Zealand, which allowed her to learn about their patient needs. Rachel says her experience has been unforgettable and would recommend the opportunity to any medical student.
“I had been introduced to the unit through the University of Otago Rural Health Student Club (Matagouri). I learned from elective reports of other trainee interns that an elective on the unit was a possibility, so I went into the placement with relatively high expectations that were fully met along the way,” Rachel says.
“I really enjoyed having an opportunity to take initiative and be a part of a team. I have entered medical school as an older medical student, having previously worked as a health professional (Speech Language Therapist), so I highly value being part of a team; there are many ways to do this on the unit. I also enjoyed meeting the people who have been working on the unit for many years and learning about their experiences. And getting to see parts of New Zealand I am less familiar with was a bonus.”
As the only student aboard the mobile surgical unit, Rachel appreciated receiving valuable practical skills, such as IV cannulation of paediatric patients and how to intubate paediatric patients. Her experience means she has been exposed to several specialities over a short period of time and this has placed more weight on certain specialities as her interest grows.
“We have very little anaesthetic training prior to our final year of medical school, and even less in the paediatric field. Having an opportunity to discuss medical and surgical careers and work-life balance with doctors in these fields was also very useful, providing me with insight into my own future potential and what the future direction of my career in medicine will be.”
She says she highly recommends taking the opportunity to work on the unit and enjoyed working in a supportive environment. “Having an opportunity to travel around more rural areas of New Zealand, talking to hospital staff and learning about the health needs, and additionally learning about intubation and other practical learning opportunities has been an unforgettable experience,” she adds.
The unit provides a unique opportunity for medical students to expand on their knowledge and skills and have a better understanding into the delivery of healthcare services to rural communities; and the challenges they face. Rachel’s invaluable experience aboard the unit was a great opportunity to gain exposure in a career in medicine and allows her to determine whether a specialty would allow her to work on the mobile surgical unit in the future. “It has also reminded me how much I enjoy being an integral part of a team, and how important that is to me as I am about to enter the medical work force.”
Carrie Bryers, Public Health Medicine Registrar – Advanced Trainee at Waitematā DHB and Auckland DHB, spent six weeks back in 2014 as a former medical student as part of her Auckland School of Medicine selective programme. Her experience on the unit made a lasting impression and the rewards went beyond just working alongside a clinical team in a perioperative environment. She also learnt about the challenges facing rural communities and the need for more doctors and nurses to work in rural practices to address New Zealand’s healthcare inequalities. Carrie says the issue of equitable access to healthcare remains a significant factor in New Zealand.
“Having medical students participate in rural settings and gain hands-on experience is crucial to promoting awareness and understanding of the challenges outside of centralised tertiary health centres. It is these future health professionals who are needed to continue to build towards solution focussed, resource savvy outcomes aimed at improving healthcare access for our rural communities,” she says.
When asked about how her time spent on the unit has prepared her for her career today, she says it has shaped it in more ways than she could have ever imagined. She recalls the time she learnt about a range of local and population health issues.
“While I was on the unit, not only was I helping with the start to end process of the surgeries, my supervisor had also arranged opportunities to have time out of the surgeries to meet with hospital managers and leaders within each community,” she begins. “I became aware of the wider impacts of health including outcomes from policy changes, resource allocation, resource limitations and how healthcare has historically and currently been delivered in New Zealand. Upon my return to hospital-based work, I started to question the way we design and deliver healthcare. I began to ‘connect the dots’ in my understanding of the barriers to healthcare access and inequities in health. This experience led me down the pathway of my career choice towards Public Health Medicine.”
At the end of each working day on the unit, the clinical team have a “team debrief” to review the activities of the day. “These debrief meetings were strong learning points as a medical student who was learning not only the surgical procedures, but understanding the community needs, challenges of rural settings, access to tertiary level care and resource needs within rural settings.”
“I recall a time speaking to a community leader, a Kaumātua in Kaikohe, which shaped my approach to practice in the years to come. We discussed the health status of his people, health inequities and how the healthcare profession could improve the delivery of health through whānau-centred care. He shared his memories of how healthcare and education use to be provided at the marae – for which he described as the ‘social centre’ for his people. I heavily reflected on this conversation and recognised the need to critically examine how we as health professionals provide care and whether this meets the needs for the community.”
There is huge concern of the scale of challenges in rural health service and Esther Maxim, Rural Health Careers Co-ordinator at NZ Rural General Practice Network says the key to a future rural health workforce comes down to developing a pipeline of rural health professionals, starting with rural youths. The Network’s rural health student network, Student of Rural Health Aotearoa (SoRHA), represents the future of rural health and wellbeing in New Zealand and provides a voice for students who are interested in improving health and wellbeing outcomes for all rural and remote New Zealanders.
SoRHA supports the Rural Health Careers Promotion programme, which aims to encourage rural school students to consider and pursue a career in health and wellbeing. “The future of rural health in New Zealand rests with our young people – it’s as simple as that,” Esther says. “Part of the problem is that we might be training enough doctors and nurses for the future, but we’re training them in the cities and they’re not moving into rural communities.”
• More than half of all GPs are aged over 52 years old. More than one third of GPs intend to retire in the next five years and 57 per cent in the next 10 years. The forecast retirement rates for rural GPs is even higher than for their urban counterparts.
• Almost 40 per cent of respondents in rural practices report a current GP vacancy
• Rural communities are twice as likely to be relying on short-term employees or contractors compared to urban centres
• Almost half of all rural GPs are now international doctors who have graduated in other countries before moving to New Zealand
• More than a quarter of all GPs (urban and rural) are experiencing burnout and our concern for the mental and physical wellbeing of rural doctors continues to increase
• Rural GPs are working longer hours than urban GPs and three quarters of rural GPs are providing after-hours and emergency care.
Read more about Mobile Health’s education programme.
Learn more about SoRHA.